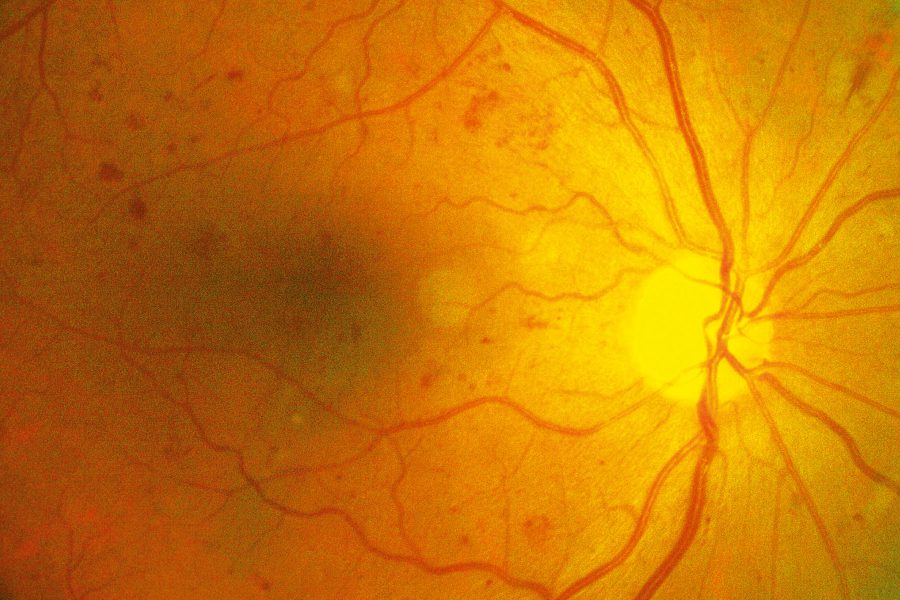
Diabetic Retinopathy Treatment
What Is Diabetic Retinopathy?
Diabetic retinopathy is an eye disorder caused by diabetes. Prolonged high blood sugar can damage the small blood vessels in the retina. It’s a serious complication that can lead to irreversible vision loss. There are two primary stages of retinopathy: the more common earlier stage is called nonproliferative, and the more serious later stage is proliferative.
Nonproliferative Diabetic Retinopathy
This is the most common type, and it occurs when small blood vessels in the eye leak. This can cause the retina to swell, as well as swelling of the macula, known as macular edema. When people with diabetes lose their vision, nonproliferative diabetic retinopathy (NDPR) is the most common reason.
In other cases, NPDR causes macular ischemia, which is when blood vessels in the retina close off, blocking blood flow to the macula. The retina can also develop small particles, or exudates, which also affect the vision.
Proliferative Diabetic Retinopathy
This more advanced stage causes the retina to grow new blood vessels, in a process called neovascularization. The new vessels are fragile and may bleed into the vitreous, which can appear as dark floaters in the vision. If the bleeding is severe enough, it can completely block the vision. Proliferative diabetic retinopathy (PDR) can also cause scar tissue from the new blood vessels. This can lead to issues with the macula or even a detached retina.
Symptoms
In its early stages, diabetic retinopathy often has no symptoms, which is why annual eye exams are so important for people with diabetes. As the condition progresses, symptoms can include:
- An increasing number of “floaters” in the vision
- Blurry vision, either constant or intermittent
- Blank or dark areas in the field of vision
- Poor night vision
- Colors appear washed out or faded
Nonproliferative diabetic retinopathy usually causes blurry vision, while proliferative diabetic retinopathy can cause dark floaters and/or blocked vision. PDR is a serious condition that can cause a loss of both central and peripheral vision.
Symptoms typically affect both eyes. Left untreated, diabetic retinopathy can eventually lead to blindness.
Causes
Diabetes is a disease that interferes with the body’s ability to use and store glucose (sugar). This can lead to high blood sugar, or too much sugar in the blood. Over time, the excess sugar causes damage to small blood vessels in the body, including the retina, which is the lining at the back of the eye.
Diagnosis
Diabetic retinopathy can be diagnosed through an eye exam or specialized tests. An ophthalmologist may put drops in the eye to dilate or widen the pupil. Then, he or she can look use a special lens to see through to the inside of the eye.
A fluorescein angiography is a procedure that shows if there are any abnormal blood vessels in the eye or if any vessels are leaking fluid or blocked. Fluorescein, a yellow dye, is injected into a vein, typically in the arm. This dye travels through the blood vessels, and then a special camera takes images of the retina.
Another way to check for diabetic retinopathy is optical coherence tomography (OCT). This imaging procedure uses a machine that scans the retina to measure the its thickness. It can also check the swelling of the macula.
Treatment
Early diagnosis and treatment of diabetic retinopathy is critical for preserving vision.
Blood Sugar Control
Maintaining good sugar control can help prevent retinopathy and vision loss in people with diabetes. Controlling blood pressure can also help maintain healthy blood vessels in the eye. Follow the recommended diet and take all prescribed diabetes or blood pressure medications.
Medications
Some medicines can help reduce swelling of the macula and slow vision loss, possibly even improving vision. Anti-VEGF medications, including Avastin, Eylea and Lucentis, and steroid may be used. Both options are given as injections into the eye.
Laser Surgery
Laser surgery can be used to shrink blood vessels and prevent regrowth, as well as sealing off leaking blood vessels and reducing retinal swelling. More than one treatment may be needed.
Vitrectomy
Treatment of advanced proliferative diabetic retinopathy may include vitrectomy. This is a surgery where an ophthalmologist removes some of the excess blood and vitreous gel from the back of the eye, as well as removing scar tissue from the retina. This enables light to reach the retina and focus correctly.
Dr. Sam Cohlmia, M.D. is a Wichita ophthalmologist and eye doctor specializing in the diagnosis and treatment of diabetic retinopathy. Call us at 316-264-8932 to schedule an appointment.