Glaucoma Diagnosis and Treatment
What is Glaucoma?
Glaucoma is a disease of the eye that affects the optic nerve. It’s the result of high pressure from excess fluid in the front of the eye, which damages the optic nerve.
Glaucoma is the second leading causes of blindness in the U.S. It’s a progressive disease, meaning vision loss gets worse over time, so early diagnosis and treatment can often prevent blindness. Most patients don’t have symptoms or vision changes until the damage is severe, so regular eye exams are critical for detecting glaucoma as soon as possible. Dr. Sam Cohlmia, M.D. is a Wichita ophthalmologist & eye doctor specializing in the diagnosis and treatment of glaucoma.
What Causes Glaucoma?
Our eyes have a built-in drainage system, called the trabecular meshwork, that maintains proper pressure. This spongy tissue is located in the drainage angle, between the iris (colored part of the eye) and cornea (clear front part of the eye). Aqueous humor, or the fluid produced inside the eye, maintains pressure and provides nutrients to the eye.
In a healthy eye, excess aqueous humor drains through the angle, out of the eye and into the circulatory system. If there’s any resistance in the trabecular meshwork, intraocular pressure (the pressure inside the eye) will gradually increase, which can result in glaucoma.
Glaucoma Types
Primary Open-Angle Glaucoma
Open-angle glaucoma is the most common type. The eye gradually stops draining fluid correctly, causing eye pressure to build up. The increased intraocular pressure then damages the ocular nerve.
Closed-Angle Glaucoma
This type of glaucoma is also referred to as arrow-angle glaucoma or angle-closure glaucoma. It happens when the iris blocks the drainage angle, and blindness can occur without immediate treatment. Chronic closed-angle glaucoma develops over time, while an acute angle-closure glaucoma attack comes on suddenly.
Other Types
In some cases, a person may have normal eye pressure levels but experience blind spots, optic nerve damage or other signs of glaucoma. This is referred to as normal tension glaucoma. At the other end of the spectrum are glaucoma suspects, who have ocular hypertension, or eye pressure that’s above the normal range. They face an increased risk of developing glaucoma and should be monitored by an ophthalmologist.
Glaucoma Symptoms
Open-angle glaucoma is painless and comes on gradually, so at first there are no symptoms or changes in vision. Blind spots will develop in the peripheral vision as the disease progresses, but the damage is usually quite severe by the time they’re noticeable.
Chronic angle-closure glaucoma doesn’t have symptoms until there’s an acute attack or the damage becomes severe. Anyone experiencing signs of an acute attack should see an ophthalmologist right away.
Symptoms of an acute closed-angle glaucoma attack:
- Sudden decreased or blurry vision
- Headache
- Severe eye or forehead pain
- Nausea
- Vomiting
- Seeing halos or rainbows
Risk Factors for Glaucoma
- Age 40 or older
- Family history of glaucoma
- African, Asian or Hispanic heritage
- Corneas with a thin center
- Chronic eye inflammation
- Farsightedness
- Nearsightedness
- Previous eye injury
- Long-term use of medicines containing steroids
- Optic nerve thinning
- Diabetes
- High blood pressure
- Migraines
- Reduced blood circulations
- Other health conditions that impact the entire body
Glaucoma Diagnosis and Testing
Glaucoma is usually first diagnosed during a complete eye exam. Although some eye doctors may screen for glaucoma by checking eye pressure, this doesn’t always find it. Glaucoma testing is typically recommended at regular intervals for anyone over age 40 and those with risk factors.
Dr. Cohlmia specializes in the glaucoma exams, testing, diagnosis and treatment, including surgery. During your exam, Dr. Cohlmia will perform tests to evaluate various aspects of your eye health:
Tonometry
Tonometry involves using eye drops to numb the eye and then using a tonometer to measure the pressure inside it. Either a puff of air or a small device will be sued to apply a small amount of pressure to the eye.
Ophthalmoscopy
An ophthalmoscopy requires the pupil of the eye to be dilated with drops so the ophthalmologist can see through it to the optic nerve. A small device is used to shine a light into the eye and magnify the optic nerve so the doctor can evaluate its shape and color.
GDx Nerve Fiber Analysis (GDx)
Cohlmia Eye Center uses a GDx (glaucoma diagnosis) instrument to scan the retina. The GDx is a relatively new test that measures the thickness of the nerve fiber layer, which is located in the back of the eye. This test can be used along with eye pressure and visual field measurements to provide a baseline and follow-up data to evaluate the existence and severity of glaucoma.
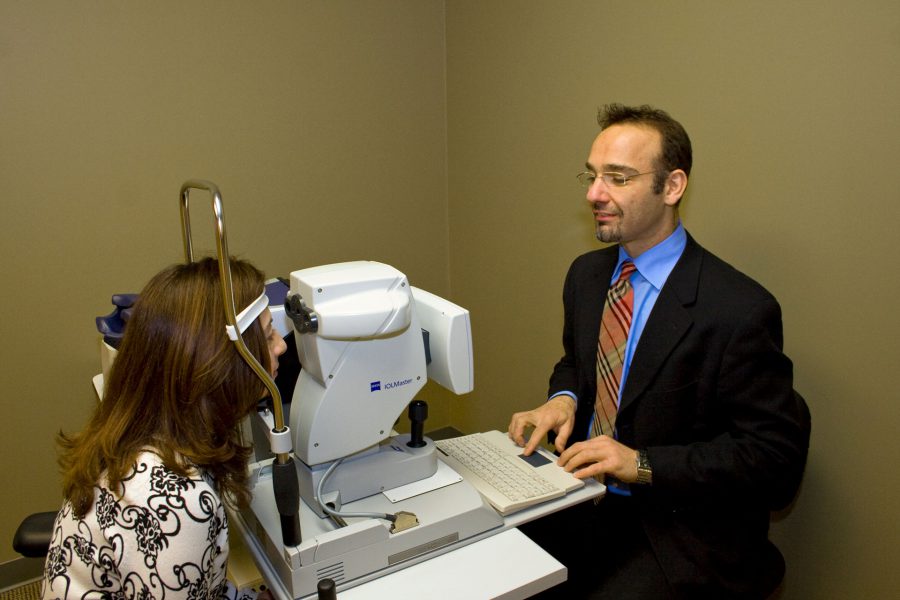
If any of the standard tests indicate high intraocular pressure or damage to the optic nerve, additional tests may be administered to confirm a glaucoma diagnosis:
Perimetry Test
To determine if your vision has been impacted by glaucoma, an ophthalmologist may perform a visual field test, known as perimetry. This test measures the ability to see a light as it moves throughout the peripheral or side vision. It will help determine if there are any blind spots that may be caused by glaucoma.
Gonioscopy
Gonioscopy is a diagnostic technique used to checks the drainage angle of the eye. Numbing drops are administered and then a mirrored contact lens is applied to the eye. The ophthalmologist can then see the angle between the cornea and the iris. If it’s blocked or closed, this could be an indication of angle-closure glaucoma. If the angle is open and wide, it could indicate open-angle glaucoma.
Pachymetry Test
A pachymeter is placed on the cornea, which is the clear layer on the front of the eye. It will measure the cornea thickness to see how it may be impacting eye pressure results.
Glaucoma Treatment
Eye damage from glaucoma is permanent and irreversible, but treatments such as medications and surgeries can help prevent further impacts on vision.
Medications
Most glaucoma medications work in one of two ways: Either reducing the production of aqueous humor or increasing its drainage through a pathway outside the trabecular meshwork. In 2017, new medications were approved by the FDA that work to target the trabecular meshwork itself.
Selective Laser Trabeculoplasty
Patients who have been diagnosed with open-angle glaucoma may be good candidates for selective laser trabeculoplasty (SLT). SLT is a quick, non-invasive laser surgery that can reduce pressure inside the eye for up to five years.
Trabeculectomy
An ophthalmologist can perform a glaucoma surgery called trabeculectomy that creates a new path for aqueous humor to drain or filter from the eye. This bubble or pocket is referred to as a filtration bleb and is usually hidden by the upper eyelid. Aqueous humor drains from the eye through a small flap that’s also created during the surgery. It then collects in the bleb where it’s absorbed by the surrounding tissue.
Glaucoma Valve Procedure
Another surgical treatment option for glaucoma involves implanting a valve or shunt to act as a small drainage tube. This drainage implant channels fluid to a reservoir created as a collection area. From there, the fluid is absorbed by the surrounding blood vessels. This treatment is typically used in cases where medications or filtering surgery have been unsuccessful. It may also be a primary procedure for patients with certain other conditions, such as:
- Neovascular Glaucoma – Associated with vascular disease of the eye (often diabetes)
- Uveitis – Acute or chronic inflammation of the eye
- Traumatic Glaucoma – Associated with injury to the eye
- Silicone Glaucoma – Resulting from silicone used to repair a detached retina
- Infantile/Juvenile Glaucoma – Associated with developmental defects of the eye
Contact us today at 316-264-8932 or schedule an appointment online for glaucoma testing or treatment.
