Macular Degeneration Treatment
What Is Age-Related Macular Degeneration?
Macular Degeneration is the leading cause of permanent vision loss in the U.S. for people over the age of 50. The eye disease typically develops as a person ages, so it’s commonly referred to as age-related macular degeneration (AMD). According to the Centers for Disease Control and Prevention, 1.8 million people have age-related macular degeneration, with another 7.3 million at a substantial risk for developing it*.
The macula is the small center area of the retina located at the back of the eye. The retina is a layer inside the eye that sends the images we see to the brain from the eye along the optic nerve. The macula focuses our central vision and allows us to see details and colors. It’s how we’re able to read words on a page or recognize people’s faces.
Macular degeneration is a disease that causes the macula to deteriorate, resulting in a loss of central vision. Although it rarely results in complete blindness, AMD can cause significant visual impairment.
There are two types of age-related macular degeneration: dry (atrophic) and wet (exudative).
Dry Age-Related Macular Degeneration
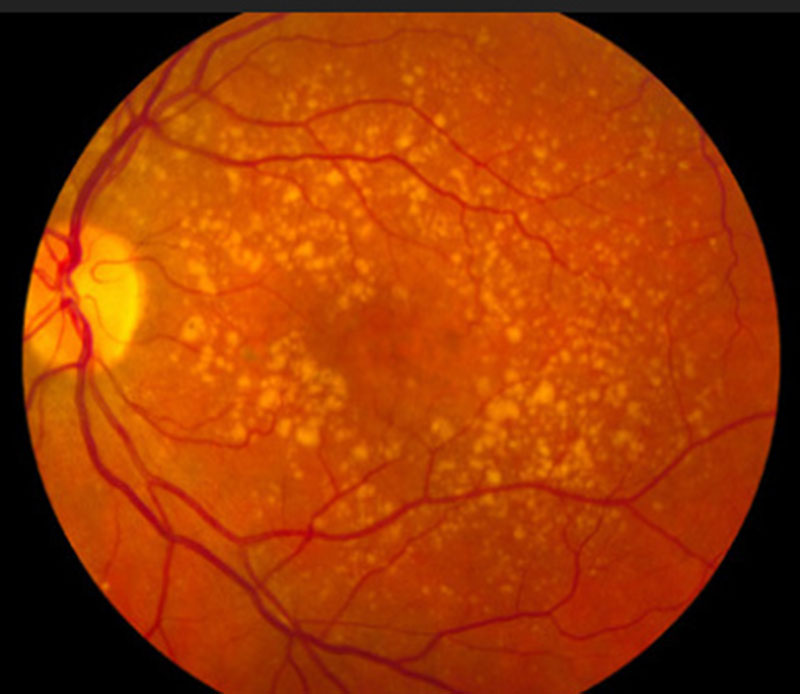
Dry AMD is the most common form, accounting for about 80% of all AMD cases. In this form, tiny yellow clumps of protein called drusen form beneath the retina and parts of the macula gradually get thinner.
Drusen alone do not cause vision loss. It’s as they grow and increase in number that a person becomes at risk for early or intermediate AMD. Central vision loss happens slowly with dry AMD, so often people don’t notice any changes in their central vision until the disease has progressed significantly .
Wet Macular Degeneration
Although less common, wet macular degeneration is far more serious than dry AMD. In this form, new, abnormal blood vessels grow under the retina. These vessels may leak blood or other fluids and can cause scarring in the macula. Vision loss happens much more quickly with wet AMD than with dry AMD and the loss is usually more severe.
Only about 10% of the people with macular degeneration have the wet form, but dry AMD can progress into wet AMD.
Stargardt Diseease
Another form of macular degeneration called Stargardt disease is a genetic disorder that’s found children and adolescents. Also known as juvenile macular degeneration, fundus flavimaculatus or Stargardt macular dystrophy, the disease is estimated to affect about 1 in every 8,000 – 10,000 people.
Macular Degeneration Stages
Age-related macular degeneration (AMD) is classified in three stages:
Early AMD: Most people don’t experience vision loss; medium-sized drusen are present
Intermediate AMD: Vision loss may or may not occur; larger drusen can be detected
Late AMD: Vision loss is noticeable
People often don’t realize they have macular degeneration until the disease has progressed. Regular visits with an ophthalmologist can detect the disease before symptoms develop.
Symptoms
Macular degeneration symptoms are generally painless and develop gradually. They can include:
- Blurry vision
- Seeing spots
- Difficulty seeing in dim light
- Distorted vision, such as straight lines appearing “wavy”
- A dark or blurry spot in the middle of the field of vision
- Colors appear less intense
- Reduced ability to see fine details
Peripheral vision is usually normal, with most symptoms affecting the central field of vision. Tasks like reading a clock or threading a needle usually become much more difficult as the disease progresses.
If you experience any of these symptoms, contact your eye doctor or ophthalmologist right away, especially if you have any of the following risk factors.
Risk Factors
While the exact cause is unknown, there are certain genetic and environmental risk factors that make a person more likely to develop age-related macular degeneration. Some can’t be controlled, such as age, race or family history. People over age 50 are more likely to get AMD, as well as those with family members who have had it. Caucasians also have a higher risk of developing macular degeneration than people from other races, and women tend to develop AMD earlier than men.
Environmental risk factors for AMD that can be controlled or avoided include:
- Eating a diet high in saturated fat
- Being overweight
- Smoking
- High blood pressure
- Heart disease
- High cholesterol
Making healthy lifestyle choices can considerably reduce the chances of getting macular degeneration.
Diagnosis
Age-related macular degeneration can be detected during an annual comprehensive eye exam. To diagnose AMD, your eye doctor or ophthalmologist will test your field of vision and use special devices to look at the inside of your eyes. Your vision professional will look for tiny yellow drusen, as well as any new or abnormal blood vessels.
First, you may be asked to look at an Amsler grid. This is just a black grid on white paper with a black dot in the middle of it. You’ll hold the grid about a foot away from your face, cover one eye and then look at the black dot in the center with your uncovered eye. This test will show you where any blank, blurry, wavy or dark spots are in your field of vision.
Your ophthalmologist will also look inside your eye through a special lens to see if there are any changes in the retina and the macula. Dilating eye drops are placed in the eye to widen your pupil and allow for a better view into the eye.
Fluorescein angiography may also be used to get a better view of your retina. Fluorescein is a yellow dye that is injected to a vein, typically in the arm, and then travels through the blood vessels. As they dye moves through the blood vessels in the eye, a special camera takes photos of the retina to see if there is any abnormal blood vessel growth beneath it.
Optical coherence tomography (OCT) also provides detailed images of both the retina and the macula using a special machine. Light waves show a cross-section of the retina, allowing an ophthalmologist to see blood and/or fluid under the retina without the use of dye.
Treatment
Unfortunately, there’s no cure for age-related macular degeneration and central vision loss is permanent. That’s why early detection is critical, because there are treatments that can slow the progression of the disease. Low vision aids, such as eyeglasses with telescoping or glare-reducing lenses, make it easier to get the most out of the remaining vision.
Dry macular degeneration treatment
At this time, the dry form of AMD doesn’t have treatment options. However, people with a large amount of drusen or serious vision loss may benefit from specific nutritional supplements. The National Eye Institute of the National Institutes of Health performed a large study called Age-Related Eye Disease Study 2 (AREDS). As a result, researchers found that AMD progression can slow when taking a daily mix of vitamins and minerals called the AREDS formula:
- Vitamin C (500 mg)
- Vitamin E (400 IU)
- Lutein (10 mg)
- Zeaxanthin (2 mg)
- Zinc (80 mg)
- Copper (2 mg)
Wet macular degeneration treatment
Although it’s not curable, there are a few treatments that can help slow the progression of wet AMD, especially when it’s diagnosed early. Anti-VEGF treatment involves using a small need to inject medications directly into the eye. The Anti-VEGF drugs reduce the number of abnormal blood vessels and slow their leaking in the retina. In some cases, laser surgery can help reduce the number of vessels in the eye and slow their leaking.
Dr. Sam Cohlmia, M.D. is a Wichita ophthalmologist and eye doctor specializing in the diagnosis and treatment of macular degeneration. Call us at 316-264-8932 to schedule an appointment.
*Source: https://www.cdc.gov/visionhealth/basics/ced/index.html